Understanding TTP
TTP is a life-threatening thrombotic microangiopathy (TMA) that requires quick diagnosis and urgent treatment. 1,2

What is TTP?
Thrombotic thrombocytopenic purpura (TTP)— A rare, life-threatening medical emergency
TTP is a rare, life-threatening thrombotic microangiopathy (TMA). There are approximately 3 cases per million people.1,2
The name thrombotic thrombocytopenic purpura describes the 3 main characteristics of the disease.
Types of TTP
Primary aTTP vs secondary aTTP2,6,7
TTP causes systemic microthrombi and consequent thrombocytopenia, hemolytic anemia, and organ ischemia. These symptoms—coupled with TTP’s rarity—can cause confusion with other TMAs, making TTP a challenge to diagnose.8-10
Signs and symptoms of aTTP include1,7-10
Suspect aTTP?
The incidence of TTP is 2 to 6 per million individuals4
aTTP primarily affects young, healthy adults13,14
If left untreated, TTP is rapidly fatal8,15-17
Even with plasma exchange therapy (PEX), mortality risk persists15,16,18
-
Joly BS, Coppo P, Veyradier A. Thrombotic thrombocytopenic purpura. Blood. 2017;129(21):2836-2846. doi:10.1182/blood-2016-10-709857
-
Arnold DM, Patriquin CJ, Nazy I. Thrombotic microangiopathies: a general approach to diagnosis and management. CMAJ. 2017;189(4):E153-E159. doi:10.1503/cmaj.160142
-
Scully M, Cataland SR, Peyvandi F, et al; HERCULES Investigators. Caplacizumab treatment for acquired thrombotic thrombocytopenic purpura. N Engl J Med. 2019;380(4):335-346. doi:10.1056/NEJMoa1806311
-
Zheng XL, Vesely SK, Cataland SR, et al. ISTH guidelines for the diagnosis of thrombotic thrombocytopenic purpura. J Thromb Haemost. 2020;18(10):2486-2495. doi:10.1111/jth.15006
-
National Institutes of Health. Congenital thrombotic thrombocytopenic purpura. Updated July 12, 2018. Accessed February 15, 2022. https://rarediseases.info.nih.gov/diseases/9430/congenital-thrombotic-thrombocytopenic-purpura
-
Sukumar S, Lämmle B, Cataland SR. Thrombotic thrombocytopenic purpura: pathophysiology, diagnosis, and management. J Clin Med. 2021;10(3):536. doi:10.3390/jcm10030536
-
Azoulay E, Bauer PR, Mariotte E, et al; Nine-i Investigators. Expert statement on the ICU management of patients with thrombotic thrombocytopenic purpura. Intensive Care Med. 2019;45(11):1518-1539. doi:10.1007/s00134-019-05736-5
-
Scully M, Hunt BJ, Benjamin S, et al; British Committee for Standards in Haematology. Guidelines on the diagnosis and management of thrombotic thrombocytopenic purpura and other thrombotic microangiopathies. Br J Haematol. 2012;158(3):323-335. doi:10.1111/j.1365-2141.2012.09167.x
-
Gallan AJ, Chang A. A new paradigm for renal thrombotic microangiopathy. Semin Diagn Pathol. 2020;37(3):121-126. doi:10.1053/j.semdp.2020.01.002
-
Tsai H-M. Pathophysiology of thrombotic thrombocytopenic purpura. Int J Hematol. 2010;91(1):1-19. doi:10.1007/s12185-009-0476-1
-
Kaplan W, Wirtz VJ, Mantel-Teeuwisse A, Stolk P, Duthey B, Laing R. Rare diseases. In: Priority Medicines for Europe and the World. 2013 Update. Chap 6.19. World Health Organization. Accessed January 27, 2022. https://www.who.int/medicines/areas/priority_medicines/MasterDocJune28_FINAL_Web.pdf?ua=1
-
Harari S, Humbert M. Ultra-rare disease: an European perspective. Eur Respir Rev. 2020;29(156):200195. doi:10.1183/16000617.0195-2020
-
Terrell DR, Williams LA, Vesely SK, Lämmle B, Hovinga JAK, George JN. The incidence of thrombotic thrombocytopenic purpura-hemolytic uremic syndrome: all patients, idiopathic patients, and patients with severe ADAMTS-13 deficiency. J Thromb Haemost. 2005;3(7):1432-1436. doi:10.1111/j.1538-7836.2005.01436.x
-
Reese JA, Muthurajah DS, Kremer Hovinga JA, Vesely SK, Terrell DR, George JN. Children and adults with thrombotic thrombocytopenic purpura associated with severe, acquired Adamts13 deficiency: comparison of incidence, demographic and clinical features. Pediatr Blood Cancer. 2013;60(10):1676-1682. doi:10.1002/pbc.24612
-
Goel R, King KE, Takemoto CM, Ness PM, Tobian AAR. Prognostic risk-stratified score for predicting mortality in hospitalized patients with thrombotic thrombocytopenic purpura: nationally representative data from 2007 to 2012. Transfusion. 2016;56(6):1451-1458. doi:10.1111/trf.13586
-
Kremer Hovinga JA, Vesely SK, Terrell DR, Lämmle B, George JN. Survival and relapse in patients with thrombotic thrombocytopenic purpura. Blood. 2010;115(8):1500-1511. doi:10.1182/blood-2009-09-243790
-
Sayani FA, Abrams CS. How I treat refractory thrombotic thrombocytopenic purpura. Blood. 2015;125(25):3860-3867. doi:10.1182/blood-2014-11-551580
-
Peyvandi F, Scully M, Kremer Hovinga JA, et al. Caplacizumab reduces the frequency of major thromboembolic events, exacerbations and death in patients with acquired thrombotic thrombocytopenic purpura. J Thromb Haemost. 2017;15(7):1448-1452. doi:10.1111/jth.13716
The burden of thrombotic thrombocytopenic purpura (TTP)
Short- and long-term implications threaten patients with aTTP
Short-term implications
An increased time at risk of microvascular thrombosis can lead to irreversible organ damage to the heart, brain, and kidneys16
Long-term implications
Long-term morbidity leads to suboptimal health-related quality of life, in both mental (anxiety, depression) and physical functioning, and potentially reduces life expectancy8-20
aTTP=acquired thrombotic thrombocytopenic purpura; CT=computed tomography; CV=cardiovascular; MI=myocardial infarction; PEX=plasma exchange; SLE=systemic lupus erythematosus; TIA=transient ischemic attack; TTP=thrombotic thrombocytopenic purpura.
- Scully M, Hunt BJ, Benjamin S, et al; British Committee for Standards in Haematology. Guidelines on the diagnosis and management of thrombotic thrombocytopenic purpura and other thrombotic microangiopathies. Br J Haematol. 2012;158(3):323-335. doi:10.1111/j.1365-2141.2012.09167.x
- Kremer Hovinga JA, Vesely SK, Terrell DR, Lämmle B, George JN. Survival and relapse in patients with thrombotic thrombocytopenic purpura. Blood. 2010;115(8):1500-1511. doi:10.1182/blood-2009-09-243790
- Sayani FA, Abrams CS. How I treat refractory thrombotic thrombocytopenic purpura. Blood. 2015;125(25):3860-3867. doi:10.1182/blood-2014-11-551580
- Goel R, King KE, Takemoto CM, Ness PM, Tobian AAR. Prognostic risk-stratified score for predicting mortality in hospitalized patients with thrombotic thrombocytopenic purpura: nationally representative data from 2007 to 2012. Transfusion. 2016;56(6):1451-1458. doi:10.1111/trf.13586
- Benhamou Y, Assié C, Boelle P-Y, et al. Development and validation of a predictive model for death in acquired severe ADAMTS13 deficiency-associated idiopathic thrombotic thrombocytopenic purpura: the French TMA Reference Center experience. Haematologica. 2012;97(8):1181-1186. doi:10.3324/haematol.2011.049676
- Chaturvedi S, Bhatia N. Predictors of survival in thrombotic thrombocytopenic purpura. Haematologica. 2013;98(5):e58. doi:10.3324/haematol.2012.079400
- Balasubramaniyam N, Yandrapalli S, Kolte D, Pemmasani G, Janakiram M, Frishman WH. Cardiovascular complications and their association with mortality in patients with thrombotic thrombocytopenic purpura. Am J Med. 2021;134(2):e89-e97. doi:10.1016/j.amjmed.2020.06.020
- Chaturvedi S, Abbas H, McCrae KR. Increased morbidity during long-term follow-up of survivors of thrombotic thrombocytopenic purpura. Am J Hematol. 2015;90(10):E208. doi:10.1002/ajh.24138
- Falter T, Schmitt V, Herold S, et al. Depression and cognitive deficits as long-term consequences of thrombotic thrombocytopenic purpura. Transfusion. 2017;57(5):1152-1162. doi:10.1111/trf.14060
- Han B, Page EE, Stewart LM, et al. Depression and cognitive impairment following recovery from thrombotic thrombocytopenic purpura. Am J Hematol. 2015;90(8):709-714. doi:10.1002/ajh.24060
- Riva S, Mancini I, Maino A, et al. Long-term neuropsychological sequelae, emotional wellbeing and quality of life in patients with acquired thrombotic thrombocytopenic purpura. Haematologica. 2020;105(7):1957-1962. doi:10.3324/haematol.2019.226423
- Alwan F, Mahdi D, Tayabali S, et al. Cerebral MRI findings predict the risk of cognitive impairment in thrombotic thrombocytopenic purpura. Br J Haematol. 2020;191(5):868-874. doi:10.1111/bjh.17126
- Hughes PA. Comprehensive care of adults with acute ischemic stroke. Crit Care Nurs Clin N Amer. 2011;23(4):661-675. doi:10.1016/j.ccell.2011.08.009
- Reed GW, Rossi JE, Cannon CP. Acute myocardial infarction. Lancet. 2017;389(10065):197-210. doi:10.1016/s0140-6736(16)30677-8
- Lau CS, Mak A. The socioeconomic burden of SLE. Nat Rev Rheumatol. 2009;5(7):400-404. doi:10.1038/nrrheum.2009.106
- Thejeel B, Garg AX, Clark WF, et al. Long-term outcomes of thrombotic microangiopathy treated with plasma exchange: a systematic review. Am J Hematol. 2016;91(6):623-630 doi:10.1002/ajh.24339
- Liu C, Kallogjeri D, Dynis M, Grossman BJ. Platelet recovery rate during plasma exchange predicts early and late responses in patients with thrombotic thrombocytopenic purpura. Transfusion. 2013(5):1096-1107. doi:10.1111/j.1537-2995.2012.03857.x
- Staley EM, Cao W, Pham HP, et al. Clinical factors and biomarkers predict outcome in patients with immune-mediated thrombotic thrombocytopenic purpura. Haematologica. 2019;104(1):166-175. doi:10.3324/haematol.2018.198275
- Kremer Hovinga JA, Coppo P, Lämmle B, Moake JL, Miyata T, Vanhoorelbeke K. Thrombotic thrombocytopenic purpura. Nat Rev Dis Primers. 2017;3:17020. doi:10.1038/nrdp.2017.20
- Deford CC, Reese JA, Schwartz LH, et al. Multiple major morbidities and increased mortality during long-term follow-up after recovery from thrombotic thrombocytopenic purpura. Blood. 2013;122(12):2023-2029. doi:10.1182/blood-2013-04-496752
The pathophysiology of thrombotic thrombocytopenic purpura (TTP)
TTP is characterized by potentially fatal systemic microthrombi1,2
TTP is caused by severely decreased activity of the ADAMTS13 enzyme. ADAMTS13 is the protease that cleaves von Willebrand factor (vWF). In patients with acquired TTP (aTTP), this deficiency is immune mediated.1
Decreased ADAMTS13 activity leads to an accumulation of ultra-large von Willebrand factor (ULvWF) multimers, which spontaneously bind to platelets and induce aggregation. This results in dangerous microthrombi that drive severe thrombocytopenia, microangiopathic hemolytic anemia, and organ ischemia.2
ADAMTS13=a disintegrin and metalloproteinase with thrombospondin type 1 motif, 13.
TTP pathophysiology
An in-depth exploration of the causes of TTP and the severe consequences of the disease.

What is the pathophysiology of aTTP?
3 Key mechanisms drive the pathophysiology of aTTP2
Normal Physiology2,3

Thrombotic Thrombocytopenic Purpura2,3
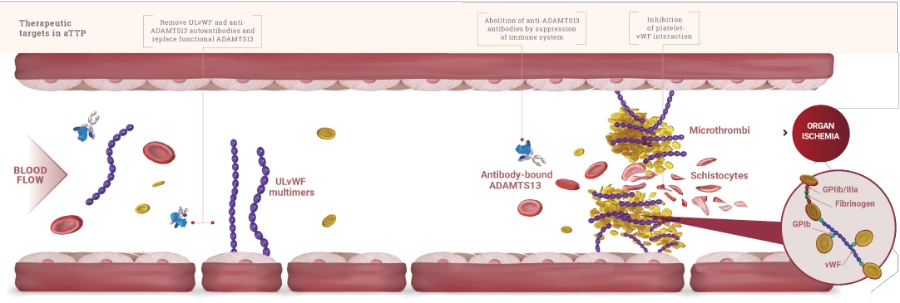
Formation of microthrombi causes2
Platelet aggregation leads to microthrombi formation, which can have fatal consequences.1,2
-
Tsai H-M. Pathophysiology of thrombotic thrombocytopenic purpura. Int J Hematol. 2010;91(1):1-19. doi:10.1007/s12185-009-0476-1
-
Joly BS, Coppo P, Veyradier A. Thrombotic thrombocytopenic purpura. Blood. 2017;129(21):2836-2846. doi:10.1182/blood-2016-10-709857
-
Saad J, Asuka E, Schoenberger L. Physiology, platelet activation. Updated May 9, 2021. Accessed November 15, 2021. https://www.ncbi.nlm.nih.gov/books/NBK482478/
Signs and symptoms of aTTP
The symptoms of aTTP are driven by microthrombi, which are unpredictable and potentially fatal1,2
Microthrombi can have serious acute and chronic consequences in TTP—putting patients at risk for devastating effects and death without urgent treatment.
Microthrombi can occur in any organ with microvessels, but the most commonly affected are3

Expert Opinion About aTTP

BR0060934_589921_Expert Roadshow video_V2_3
Signs and symptoms of acquired thrombotic thrombocytopenic purpura (aTTP) include1,4,5
of TTP episodes result in ischemia due to platelet aggregation in the microcirculation of the brain.3
The consequences of microthrombi can be severe, with TTP potentially resulting in acute thromboembolic events such as1,2,4
Consequences can also be long term
-
Joly BS, Coppo P, Veyradier A. Thrombotic thrombocytopenic purpura. Blood. 2017;129(21):2836-2846. doi:10.1182/blood-2016-10-709857
-
Goel R, King KE, Takemoto CM, Ness PM, Tobian AAR. Prognostic risk-stratified score for predicting mortality in hospitalized patients with thrombotic thrombocytopenic purpura: nationally representative data from 2007 to 2012. Transfusion. 2016;56(6):1451-1458. doi:10.1111/trf.13586
-
Moake JL. Thrombotic thrombocytopenic purpura: the systemic clumping “plague.” Annu Rev Med. 2002;53:75-88. doi:10.1146/annurev.med.53.082901.103948
-
Scully M, Hunt BJ, Benjamin S, et al; British Committee for Standards in Haematology. Guidelines on the diagnosis and management of thrombotic thrombocytopenic purpura and other thrombotic microangiopathies. Br J Haematol. 2012;158(3):323-335. doi:10.1111/j.1365-2141.2012.09167.x
-
Azoulay E, Bauer PR, Mariotte E, et al; Nine-i Investigators. Expert statement on the ICU management of patients with thrombotic thrombocytopenic purpura. Intensive Care Med. 2019;45(11):1518-1539. doi:10.1007/s00134-019-05736-5

.jpg/jcr:content/jcr_content%20(15).jpg)
